As I mentioned in one of my earlier blogs, I was hospitalized just a few days after my college graduation due to a severe flare of Ulcerative Colitis. I had been wanting a puppy for quite some time, and thought that this hospitalization was the perfect opportunity to guilt my Dad into buying me one. "Those dogs need help just like I need help right now, Dad," I would say. "I would not just be saving a dog, the dog would be saving me too." While in the middle of one of my infamous guilt trips, my middle-aged and puppy-eyed nurse who just happened to suffer from Crohn's disease herself chimed in, "I saved a dog three years ago and I have been in remission ever since," she turned to my Dad, "haven't you ever heard of pet therapy?" That sealed the deal.
I convinced my father to stop by North Shore Animal League, the nation's largest no-kill shelter, immediately after my discharge from the hospital. With my hospital bracelet still attached and an indelible smile painted on my face, I walked as quickly as I could into the shelter. A small, 10-week old beagle puppy caught my eye and I was sure she was the one. I reached down to save her from her cage, only to find that I was too weak to lift the 6-pound pup. "I think we'll have to come back another time," my father lamented. I huffed and I puffed, but I ultimately relinquished my hopes of bringing home a new member of the family. For now.
It was just a few weeks later when we returned to North Shore Animal League. It was on this trip that I met the love of my life, la Figlia Mia. While I can't say that I have been in remission ever since bringing Figlia home, I can say that I am able to cope with and manage my disease at a level that I hadn't been able to before she became a part of my life. We walk together, which helps me to recover. We play together, which gives me an always-effective dose of laughter. Whenever I cry, she licks away my tears and whenever I laugh she is there to join in my happiness. She needs her belly rubbed every morning, even when I am too sick to get out of my bed, and it is perhaps this fact more than any other that I enjoy; knowing that even when I am relying on others, someone still needs me. Figlia may not be able to cure my disease or prevent side effects and surgical complications, but she gives me something much more important; unconditional love.
As I sit here with my canine friend, 8.5 weeks post-op and 3.5 weeks pre-op (though my second surgery date is yet to be confirmed), I question whether I want to go through another surgery, another hospitalization, and another recovery. My ileostomy has allowed me the freedom, peace of mind, and health that I have been unable to experience in nearly a decade. Yes, it leaks on occasion. Yes, it is a pain to change the ostomy. And, no, I am still not used to seeing my intestine sticking through my abdomen. But would I have it any other way? No. I am so lucky to have my body back, to have my health back and I am not so sure I want to risk complicating that with another procedure. Will I go through with it? Probably, because bag or no bag, Figlia will love me just the same.
Monday, May 30, 2011
Friday, May 20, 2011
How it Feels to be 7-weeks Post-Op
I realized it's been a few weeks since I have given a status update on my condition. I saw Dr. Procaccino (my surgeon) a week ago for a follow-up sigmoidoscopy to see how the J-Pouch is healing. While this was one of the more unpleasant procedures I have had in a while (think raw scar tissue from a freshly-created organ), the prognosis was very promising. The J-Pouch is looking "perfect" as Dr. Procaccino said, and we will be doing another follow-up procedure the first week of June to determine whether the J-Pouch is ready to be used. This will entail injecting dye into the J-Pouch and then a subsequent X-Ray to show whether the J-Pouch has any leaks. If all goes well, I will be ready for Surgery #2 (from a colorectal point of view).
I also saw my vascular surgeon (Dr. Krisnasastry) last week for a follow-up on the PVT (blood clots). I begged him to let me have my next surgery at the end of June since I want to be streamlined and bag-less for my October wedding. He found that funny. "We all wish that things would go perfectly, but sometimes they don't," he reminded me with a chuckle. Though he didn't make any promises, he did make a few concessions. He moved up the follow-up CT Scan to the first week of June and said if the PVTs showed any sign of resolution he would allow me to have my next surgery at the end of June. He added that there was almost no chance they would be completely resolved or recanalized, as PVTs take at least three months to begin this process. However, he would not be looking for complete resolution at this point and he would feel confident going into my next procedure as long as the PVTs looked better than they did in the first CT Scans. The issue of whether I will remain on the Coumadin for 3 months, 6 months, or indefinitely will also be determined at this juncture.
Physically, I am feeling great. Dr. Procaccino said to me last week, "I told you that you would be feeling well after 6 weeks!" I said, "Hell, I was feeling great at 4!" I have been very happy with my recovery from this first surgery, but I must say it takes work. I have been walking every single day at least 1.5 miles since week 4 (I was told by my doctors that walking will speed recovery). I have been scrupulous about not lifting anything heavy (more than 5-10lbs.) and have made sure to get a lot of sleep. I still have minimal pain and discomfort in my abdomen and I feel considerably more fatigued at the end of the day than I did pre-op, but these are my only complaints. Overall, I feel much healthier and happier than I did living with U.C. and, despite the complications from the surgery, I am very happy that I followed through with the panproctocolectomy.
As far as our CCFA Benefit Concert goes, we are hard at work pulling together the details and are on the brink of confirming a venue. I'll keep you all on your toes, but hope to reveal the location by this weekend or early next week!
I also saw my vascular surgeon (Dr. Krisnasastry) last week for a follow-up on the PVT (blood clots). I begged him to let me have my next surgery at the end of June since I want to be streamlined and bag-less for my October wedding. He found that funny. "We all wish that things would go perfectly, but sometimes they don't," he reminded me with a chuckle. Though he didn't make any promises, he did make a few concessions. He moved up the follow-up CT Scan to the first week of June and said if the PVTs showed any sign of resolution he would allow me to have my next surgery at the end of June. He added that there was almost no chance they would be completely resolved or recanalized, as PVTs take at least three months to begin this process. However, he would not be looking for complete resolution at this point and he would feel confident going into my next procedure as long as the PVTs looked better than they did in the first CT Scans. The issue of whether I will remain on the Coumadin for 3 months, 6 months, or indefinitely will also be determined at this juncture.
Physically, I am feeling great. Dr. Procaccino said to me last week, "I told you that you would be feeling well after 6 weeks!" I said, "Hell, I was feeling great at 4!" I have been very happy with my recovery from this first surgery, but I must say it takes work. I have been walking every single day at least 1.5 miles since week 4 (I was told by my doctors that walking will speed recovery). I have been scrupulous about not lifting anything heavy (more than 5-10lbs.) and have made sure to get a lot of sleep. I still have minimal pain and discomfort in my abdomen and I feel considerably more fatigued at the end of the day than I did pre-op, but these are my only complaints. Overall, I feel much healthier and happier than I did living with U.C. and, despite the complications from the surgery, I am very happy that I followed through with the panproctocolectomy.
As far as our CCFA Benefit Concert goes, we are hard at work pulling together the details and are on the brink of confirming a venue. I'll keep you all on your toes, but hope to reveal the location by this weekend or early next week!
Tuesday, May 17, 2011
Benefit for CCFA!
Progress has been made regarding our CCFA( Crohns & Colitis Foundation of America ) benefit concert, featuring Iris' band Roads and my brother Mark's band The Alphabets. Our tentative date is Sunday, August 14th...so please put this on your calendar! We will be booking a venue sometime this week and the concert will be hosted either on Long Island or in Manhattan. The official location will be revealed in my next blog, but we have quite a few exciting venues that we are considering!
If anyone is interested in sponsoring or assisting with the event, any help would be warmly welcomed and sincerely appreciated! I can be contacted by email : kboccard@gmail.com
We are very excited about the fundraiser and we hope all can attend! Spread the word!
If anyone is interested in sponsoring or assisting with the event, any help would be warmly welcomed and sincerely appreciated! I can be contacted by email : kboccard@gmail.com
We are very excited about the fundraiser and we hope all can attend! Spread the word!
Sunday, May 15, 2011
Convalescent Ruminations
I met a good childhood friend for lunch earlier in the week and he asked how my fiance Billy has been handling my surgery and how he coped with my disease. I responded by telling him how incredible Billy is and how he has been my rock (not to be cliche). My friend reminded me at this point how lucky I was to have such a guy and gently mentioned how most guys wouldn't be so strong and so faithful, how many people run away from challenges such as these and abandon those they most love. "Maybe people just have bad hearts," he concluded, "but I'm just not sure." We parted ways at this point, but his words stuck with me.
Truth is, I AM lucky to have such a steady, caring and patient man to share the rest of my life with. I adamantly believe that it is more challenging and difficult to be the caretaker of a sick loved one than it is to be the one who is ill. Billy and I are both so lucky to finally be rid of this disease and we are both looking forward to our new life together. Upon completing my surgery, Dr. Procaccino met with my parents and Billy while I was in the recovery room. He turned to Billy and said, "Everything went perfectly. Her colon was very, very diseased and I want you to know that she made the right choice. Your life together is going to be so much better because she made this decision." But this wasn't a choice I could have made alone. I have been incredibly lucky to have such a strong and reliable support network of not only Billy, my parents and my brother, but also my friends, family and even other Crohn's and Colitis patients that have been able to personally relate to me. Knowing that Billy would be by my side no matter what, having my Mom and Dad and brother next to my side 24/7 at the hospital, talking to several other panproctocolectomy patients that assured me the grass was greener without a colon. I couldn't have made this life-changing decision without each of them.
The grass is certainly greener, the sun is brighter, and the sky is bluer. Maybe it's because I am finally able to see the grass and look at the sky because I no longer live in a bathroom. But it's also because living with this disease and beating the constant challenges it has thrown my way has taught me of the delicacy of life and has endowed me with a much greater appreciation for my health than I ever could have hoped to experience if I hadn't stumbled into this hurdle called U.C. For all you Crohn's and Colitis patients out there, take advantage of the sunny days and don't lose hope during the cloudy ones. The rain can only last so long.
Truth is, I AM lucky to have such a steady, caring and patient man to share the rest of my life with. I adamantly believe that it is more challenging and difficult to be the caretaker of a sick loved one than it is to be the one who is ill. Billy and I are both so lucky to finally be rid of this disease and we are both looking forward to our new life together. Upon completing my surgery, Dr. Procaccino met with my parents and Billy while I was in the recovery room. He turned to Billy and said, "Everything went perfectly. Her colon was very, very diseased and I want you to know that she made the right choice. Your life together is going to be so much better because she made this decision." But this wasn't a choice I could have made alone. I have been incredibly lucky to have such a strong and reliable support network of not only Billy, my parents and my brother, but also my friends, family and even other Crohn's and Colitis patients that have been able to personally relate to me. Knowing that Billy would be by my side no matter what, having my Mom and Dad and brother next to my side 24/7 at the hospital, talking to several other panproctocolectomy patients that assured me the grass was greener without a colon. I couldn't have made this life-changing decision without each of them.
The grass is certainly greener, the sun is brighter, and the sky is bluer. Maybe it's because I am finally able to see the grass and look at the sky because I no longer live in a bathroom. But it's also because living with this disease and beating the constant challenges it has thrown my way has taught me of the delicacy of life and has endowed me with a much greater appreciation for my health than I ever could have hoped to experience if I hadn't stumbled into this hurdle called U.C. For all you Crohn's and Colitis patients out there, take advantage of the sunny days and don't lose hope during the cloudy ones. The rain can only last so long.
Wednesday, May 11, 2011
Remicade & The Super-Bug
I had my first infusion of Remicade in December of 2009. I was still on Prednisone at this point and had just finished a two-month course of Flagyl and Vancomycin, antibiotics that were used in tandem to treat a resilient C-Difficil infection. C-Difficil is a bacterial infection that causes symptoms that are virtually identical to U.C. symptoms and therefore often go undetected for dangerously long periods of time in IBD patients. Ulcerative Colitis and Crohn's patients are the only people on earth who are able to develop spontaneous C.Difficil infections as they are otherwise only caused by antibiotics or are transmitted, generally in a hospital setting. This was not my first encounter with C.Difficil, but now that I am cured of Ulcerative Colitis and no longer have a colon, I can safely say that it was my last.
Once the C.Diff was cleared I was able to "safely" begin my treatments with Remicade. Remicade is a TNF-blocker (tumor necrosis factor) that is administered via I.V. over the course of several hours. U.C. patients have elevated levels of TNF, a cytokine that causes inflammation. It functions by inhibiting the TNF response in the body's immune system. Remicade can be a wonder drug, and it allowed me to live blissfully in remission for the longest period of time in 9 years. But users should be wary. While fairly rare, Remicade has been found to cause leukemia, lymphoma, lupus, congestive heart failure, and other serious diseases and side effects. It has been more commonly linked with respiratory illnesses, such as tuberculosis, and so Remicade patients must be tested for T.B. regularly. Serious allergic reactions to Remicade are not exceedingly rare and chronic sinus infections and mild bronchial infections are quite common. Because of the considerable dangers of using this drug, Remicade is only administered as a last-ditch effort before surgery becomes imminently necessary.
On a more practical note, Remicade is simply a pain. Because it is administered intravenously, you become a prisoner to a hospital or clinic's 9-5, Monday-Friday schedule. If you are a working woman/man, this can become quite taxing. Infusions are generally given every 6-8 weeks (initially it is spaced every 2 weeks, then 4 weeks until you reach a therapeutic level). I personally found it difficult having to take a half or full day off of work this frequently.
Around December of 2010 my U.C. became symptomatic yet again. I had hoped that my upcoming Remicade infusion in January would set everything straight. It didn't. I became increasingly worse over the next eight weeks until my next infusion in March of 2011. At this point I was feeling very run down as it had been over two months of active U.C. symptoms. I knew that a lot depended on this infusion. If it didn't work, I would be back on Prednisone at best, and in surgery at worst. About twenty minutes into the infusion I felt like I was suddenly hit with a ton of bricks. I went into anaphylactic shock. Within seconds a team of nurses and doctors were at my side. They immediately stopped the Remicade infusion and administered Benadryl into the I.V. Within minutes I was stabilized. When normal breathing returned it was quickly accompanied by an almost convulsive bout of crying. I was scared. The first thing I was able to think of was the fact that this was the end of the road for me. I was going to need surgery. I pictured the ostomy bag on my side, which I knew was imminent. I thought of the life-threatening allergic reaction I had just endured. I thought of the fact that I had just subjected my body to nine years of risky medicinal treatments and had suffered from this disease for almost a decade...and for what? I had lost this battle.
Surgeons will only perform a panproctocoletomy for four reasons: 1. the patient has colon cancer that is unresponsive to chemotherapy or radiation treatments 2. in pediatric cases where a Crohn's or U.C. patient is unable to grow because of severe vitamin deficiencies 3. toxic megacolon 4. a U.C. patient has run through all possible medicinal treatment options. While I appreciate this conservative approach to surgery, I can't help but be somewhat critical of it. If I had undergone these surgeries nine years ago, would I now have healthy kidneys? Would my hands be free of dysplasia? Would I not have to worry about all the long-term effects of prolonged steroid use? What would I have accomplished or experienced in all those years I was so ill?
These questions will probably always be lingering in the back of my mind. There is a fine line between optimism and denial, and I do not want to breach it. For now, I am focusing on how lucky I am to have had this surgery, how lucky I am to be alive, and how excited I am by all the thing I will accomplish and experience in the future because I was able to have these surgeries.
Once the C.Diff was cleared I was able to "safely" begin my treatments with Remicade. Remicade is a TNF-blocker (tumor necrosis factor) that is administered via I.V. over the course of several hours. U.C. patients have elevated levels of TNF, a cytokine that causes inflammation. It functions by inhibiting the TNF response in the body's immune system. Remicade can be a wonder drug, and it allowed me to live blissfully in remission for the longest period of time in 9 years. But users should be wary. While fairly rare, Remicade has been found to cause leukemia, lymphoma, lupus, congestive heart failure, and other serious diseases and side effects. It has been more commonly linked with respiratory illnesses, such as tuberculosis, and so Remicade patients must be tested for T.B. regularly. Serious allergic reactions to Remicade are not exceedingly rare and chronic sinus infections and mild bronchial infections are quite common. Because of the considerable dangers of using this drug, Remicade is only administered as a last-ditch effort before surgery becomes imminently necessary.
On a more practical note, Remicade is simply a pain. Because it is administered intravenously, you become a prisoner to a hospital or clinic's 9-5, Monday-Friday schedule. If you are a working woman/man, this can become quite taxing. Infusions are generally given every 6-8 weeks (initially it is spaced every 2 weeks, then 4 weeks until you reach a therapeutic level). I personally found it difficult having to take a half or full day off of work this frequently.
Around December of 2010 my U.C. became symptomatic yet again. I had hoped that my upcoming Remicade infusion in January would set everything straight. It didn't. I became increasingly worse over the next eight weeks until my next infusion in March of 2011. At this point I was feeling very run down as it had been over two months of active U.C. symptoms. I knew that a lot depended on this infusion. If it didn't work, I would be back on Prednisone at best, and in surgery at worst. About twenty minutes into the infusion I felt like I was suddenly hit with a ton of bricks. I went into anaphylactic shock. Within seconds a team of nurses and doctors were at my side. They immediately stopped the Remicade infusion and administered Benadryl into the I.V. Within minutes I was stabilized. When normal breathing returned it was quickly accompanied by an almost convulsive bout of crying. I was scared. The first thing I was able to think of was the fact that this was the end of the road for me. I was going to need surgery. I pictured the ostomy bag on my side, which I knew was imminent. I thought of the life-threatening allergic reaction I had just endured. I thought of the fact that I had just subjected my body to nine years of risky medicinal treatments and had suffered from this disease for almost a decade...and for what? I had lost this battle.
Surgeons will only perform a panproctocoletomy for four reasons: 1. the patient has colon cancer that is unresponsive to chemotherapy or radiation treatments 2. in pediatric cases where a Crohn's or U.C. patient is unable to grow because of severe vitamin deficiencies 3. toxic megacolon 4. a U.C. patient has run through all possible medicinal treatment options. While I appreciate this conservative approach to surgery, I can't help but be somewhat critical of it. If I had undergone these surgeries nine years ago, would I now have healthy kidneys? Would my hands be free of dysplasia? Would I not have to worry about all the long-term effects of prolonged steroid use? What would I have accomplished or experienced in all those years I was so ill?
These questions will probably always be lingering in the back of my mind. There is a fine line between optimism and denial, and I do not want to breach it. For now, I am focusing on how lucky I am to have had this surgery, how lucky I am to be alive, and how excited I am by all the thing I will accomplish and experience in the future because I was able to have these surgeries.
Monday, May 9, 2011
Mercaptopurine (6MP)
My experience with 6MP has a bit of a curious storyline. I first used this medication as a senior in high school, less than a year from the time of my diagnosis. The frequent blood tests were the only complaint I might have made about it since I would have to occasionally miss or be late for some after-school activities. I was very secretive about my disease at this point as I didn't want most people to know that I had a disease that involved frequent and bloody bowel movements. I was sure that no boy or man would ever be interested in me if they knew about any of that. But, having 81 absences in my senior year and taking the AP exams in a "special" room with extra allotted time to allow for my frequent trips to the bathroom was not an easy thing to hide. Nor was my two month-long absence from school when I was initially diagnosed, or my tardiness for after school activities to allow for frequent trips to doctors or for the 6MP blood tests.
I took myself off of 6MP when I went to college as I had experienced the longest remission yet (a little under 1 year) and, quite frankly, the drug scared me. It was only when I began experiencing more frequent flares that I was prescribed 6MP again. It worked. For a while. I had frequent mild flares, including a fairly severe one while studying abroad in Rome. At the end of my senior year of college I had a very severe flare and was hospitalized for a week just 2 days after my graduation. After moving to Washington D.C., my gastroenterologist down there (Dr. Ginsberg) noticed the sudden appearance of around 25 small moles on the palms of my hands. He asked how long they had been there. I told him the appeared a few months prior. He and a team of dermatologists ran some tests and determined that they were dysplastic nevi and were a rare side effect of 6MP.
Because of a strong family history of melanoma (both my mother and father and quite a few of their siblings), combined with the fact that the 6MP was losing its efficacy and failing to keep my UC under control, both my D.C. gastroenterologist and my primary gastroenterologist in NY decided to take me off of the 6MP, at first thinking they could just treat my flares with Prednisone as I only had one more class of drugs to try before surgery would be on the table. They quickly found that my disease was too severe to treat with intermittent steroids and after another week-long hospital stay and a fight with a C. Difficile, I was faced with my last hope to save my colon. I was put on a TNF-blocker called Remicade....
I took myself off of 6MP when I went to college as I had experienced the longest remission yet (a little under 1 year) and, quite frankly, the drug scared me. It was only when I began experiencing more frequent flares that I was prescribed 6MP again. It worked. For a while. I had frequent mild flares, including a fairly severe one while studying abroad in Rome. At the end of my senior year of college I had a very severe flare and was hospitalized for a week just 2 days after my graduation. After moving to Washington D.C., my gastroenterologist down there (Dr. Ginsberg) noticed the sudden appearance of around 25 small moles on the palms of my hands. He asked how long they had been there. I told him the appeared a few months prior. He and a team of dermatologists ran some tests and determined that they were dysplastic nevi and were a rare side effect of 6MP.
Because of a strong family history of melanoma (both my mother and father and quite a few of their siblings), combined with the fact that the 6MP was losing its efficacy and failing to keep my UC under control, both my D.C. gastroenterologist and my primary gastroenterologist in NY decided to take me off of the 6MP, at first thinking they could just treat my flares with Prednisone as I only had one more class of drugs to try before surgery would be on the table. They quickly found that my disease was too severe to treat with intermittent steroids and after another week-long hospital stay and a fight with a C. Difficile, I was faced with my last hope to save my colon. I was put on a TNF-blocker called Remicade....
Saturday, May 7, 2011
Prednisone: My Best Friend and Worst Enemy
I know many people have had experiences with Prednisone as it is a drug used for many, many different ailments. There are generally two different ways Prednisone is used: 1. a short term treatment of >25 mg. for 1-2 weeks. 2. a long term treatment of <25 mg. that is generally prescribed for many months. I have experienced both and all I can say is these two different courses of treatment with Prednisone seem like two entirely different drugs.
Generally, in the case of U.C., Prednisone is used in higher doses, for a longer period of time. For example, I would generally show very little to no relief of symptoms if prescribed less than 60mg. As a side note, if you are on Prednisone for longer than 2 weeks, your own adrenal system shuts down and relies on the Prednisone entirely. So for those of you that hate this drug as much as I do, please know that it is VERY important that you follow doctor's orders and wean off of this drug exactly as they instruct. Prednisone cannot be used in large doses for the long term as it is a very dangerous drug when used in such high doses, with many, many side effects which is why Prednisone was only used as a temporary treatment to get bad flares of U.C. under control. Prednisone is a drug that I was on many, many times throughout the last 9 years and I have been on it in small doses, high doses, and even intravenously. In fact, I was on Prednisone so many times that in the last year or two, it stopped having any therapeutic effect, even when given doses of 100mg or more.
As a teenager and young woman suffering from U.C. and taking this medication, the side effects from Prednisone often became even more difficult to deal with than the disease itself. My face and body would be invaded with what one dermatologist called "the worst case of acne from Prednisone [he had] ever seen in [his] career" (note: he was 85). I would gain weight at a very rapid pace, even if I wasn't eating much, although the Prednisone gives you a ravenous appetite. Last year after a week-long hospitalization I went from 120 lbs. to 144lbs. in just two weeks from the high doses of Prednisone. If on high enough doses, I would have excruciating joint pains, especially in my knees and until I would be on less than 20mg, sleeping for any amount of time was out of the question. In high school I took the SAT when on high doses of Prednisone and after not sleeping for several weeks and scored much lower than expected, so I inquired with the SAT company as to what happened. They wrote back and said I didn't fill out two pages worth of questions on the scantron! Thank god I was able to retake them!
The side effects I mentioned above are, unfortunately, experienced by many people given high doses of Prednisone. On the bright side, Prednisone worked to put my U.C. symptoms in remission or at least assuage the pain and/or symptoms and was effective as a treatment for me for many years. One thing I must say to any of you out there that are frequently using Prednisone in high doses is PLEASE be careful! This is a very dangerous drug that should be used exactly as prescribed. For those of you that find you are on Prednisone frequently for U.C., I would discuss other maintenance treatment options as Prednisone cannot be used in the long term.
I took my last dose of Prednisone on Sunday, April 10, 2011. Putting this drug behind me has undoubtedly been one of the best outcomes of going through the panproctocolectomy!!
The CCFA (Crohn's and Colitis Foundation of America) is constantly raising funds and conducting cutting-edge research in order to find more effective and safer treatment options for those suffering from these diseases. My wonderful Aunt Regina is currently fundraising for the CCFA's 1/2 marathon in Kona, Hawaii that takes place on June 26. If anyone is interested in making a tax-deductable donation to the CCFA to fund research and help Regina reach her fundraising goals, please follow the following link: http://www.active.com/donate/
Thank you in advance to anyone who decides to donate and please, as always, reach out to me if you have any questions about Prednisone or if you know anyone (especially a youngster) who just needs someone to talk to. It can be very emotionally-distressing to be on Prednisone and just having someone to talk to can help!
Generally, in the case of U.C., Prednisone is used in higher doses, for a longer period of time. For example, I would generally show very little to no relief of symptoms if prescribed less than 60mg. As a side note, if you are on Prednisone for longer than 2 weeks, your own adrenal system shuts down and relies on the Prednisone entirely. So for those of you that hate this drug as much as I do, please know that it is VERY important that you follow doctor's orders and wean off of this drug exactly as they instruct. Prednisone cannot be used in large doses for the long term as it is a very dangerous drug when used in such high doses, with many, many side effects which is why Prednisone was only used as a temporary treatment to get bad flares of U.C. under control. Prednisone is a drug that I was on many, many times throughout the last 9 years and I have been on it in small doses, high doses, and even intravenously. In fact, I was on Prednisone so many times that in the last year or two, it stopped having any therapeutic effect, even when given doses of 100mg or more.
As a teenager and young woman suffering from U.C. and taking this medication, the side effects from Prednisone often became even more difficult to deal with than the disease itself. My face and body would be invaded with what one dermatologist called "the worst case of acne from Prednisone [he had] ever seen in [his] career" (note: he was 85). I would gain weight at a very rapid pace, even if I wasn't eating much, although the Prednisone gives you a ravenous appetite. Last year after a week-long hospitalization I went from 120 lbs. to 144lbs. in just two weeks from the high doses of Prednisone. If on high enough doses, I would have excruciating joint pains, especially in my knees and until I would be on less than 20mg, sleeping for any amount of time was out of the question. In high school I took the SAT when on high doses of Prednisone and after not sleeping for several weeks and scored much lower than expected, so I inquired with the SAT company as to what happened. They wrote back and said I didn't fill out two pages worth of questions on the scantron! Thank god I was able to retake them!
The side effects I mentioned above are, unfortunately, experienced by many people given high doses of Prednisone. On the bright side, Prednisone worked to put my U.C. symptoms in remission or at least assuage the pain and/or symptoms and was effective as a treatment for me for many years. One thing I must say to any of you out there that are frequently using Prednisone in high doses is PLEASE be careful! This is a very dangerous drug that should be used exactly as prescribed. For those of you that find you are on Prednisone frequently for U.C., I would discuss other maintenance treatment options as Prednisone cannot be used in the long term.
I took my last dose of Prednisone on Sunday, April 10, 2011. Putting this drug behind me has undoubtedly been one of the best outcomes of going through the panproctocolectomy!!
The CCFA (Crohn's and Colitis Foundation of America) is constantly raising funds and conducting cutting-edge research in order to find more effective and safer treatment options for those suffering from these diseases. My wonderful Aunt Regina is currently fundraising for the CCFA's 1/2 marathon in Kona, Hawaii that takes place on June 26. If anyone is interested in making a tax-deductable donation to the CCFA to fund research and help Regina reach her fundraising goals, please follow the following link: http://www.active.com/donate/
Thank you in advance to anyone who decides to donate and please, as always, reach out to me if you have any questions about Prednisone or if you know anyone (especially a youngster) who just needs someone to talk to. It can be very emotionally-distressing to be on Prednisone and just having someone to talk to can help!
Thursday, May 5, 2011
Why 5-ASA is History
I have dedicated this blog thus far to my experiences in the last 5 weeks and to the panproctocolectomy surgery. While this period of time has certainly been a challenge, it has been just a small jigsaw in a much larger puzzle. Since I have been on approximately 5 different classes of drug treatments over the last 9 years, I would like to dedicate my next 5 blog entries to discussion of my experiences with each of them.
I was first diagnosed with Ulcerative Colitis via colonoscopy in 2002 by my pediatric gastroenterologist, Dr. Markowitz at North Shore University Hospital. I was very sick at the time of my diagnosis and so I was put on 60 mg. of Prednisone (a corticosteroid) and was also prescribed Asacol, a 5-ASA or mesalamine drug. I would take 16 Asacol pills daily (4 pills, 4 times a day), though thanks to the CCFA and strides made in the field of research, Asacol was recently condensed and is now given as 1 pill, once per day. I was also given prescription Iron to treat my anemia and a prescribed form of Folic Acid as Ulcerative Colitis patients are known to have chronically-low Folic Acid levels.
Thanks to Prednisone, I was able to achieve remission from U.C. within two weeks of my diagnosis, although I had lost 20 pounds and was very weak so it took quite a bit longer to gain my strength back. I was slowly weaned off of the Prednisone over a period of 4 months and felt well for that length of time. Unfortunately, once I was off the Prednisone, the Asacol was unable to keep me in remission on its own and so my doctor added Colazal (Balzalazide), another 5-ASA agent to my regimen. This added another 10 pills daily, and I believe at this point I was up to around 31 pills/day. The Colazal didn't work. Instead of taking me off of the 5-ASA agents, another drug was added. At this point (about 8 months after my diagnosis) I was given 6MP (mercaptopurine), a drug used more often in the treatment of leukemia that required biweekly blood tests to assure my white blood cell count remained in a healthy range. As an important side note, Ulcerative Colitis is an autoimmune disease, meaning your immune system attacks itself. Therefore, the treatment for Ulcerative Colitis necessarily requires the suppression of your immune system, and so these treatments lower your white blood cell count and inhibit your body's natural ability to fight off infections. I was able to achieve intermittent remission with 6MP, but was left on the 5-ASA agents for 3 years.
During a routine visit to my gastroenterologist in Maine while I was in college, my doctor found high amounts of protein in my urine which is symptomatic of compromised kidney function. I was immediately sent to a nephrologist who deduced that the damage done to my kidneys was caused by the 5-ASA agents. Now, I must explain that this is a rare complication of 5-ASA drugs, though it does happen. 5-ASA are the most mild and least risky treatments used for U.C. and those that are able to obtain remission on 5-ASA agents with no serious side effects are very lucky.
For me, 5-ASA agents were eternally taken off the radar. I was no longer a candidate for them, but because of their very limited efficacy in treatment of my U.C., I did not find this news to be particularly troublesome. I was now onto a cocktail of 6MP and high doses of Prednisone (the Prednisone was taken sporadically, but I spent more time on them than off).
In conclusion, 5-ASA drugs are relatively harmless in comparison to other U.C. treatment options and if they work for you...stick with them!
And, oh, I turned those pictures around from yesterday as I know it was irking some of you!
I was first diagnosed with Ulcerative Colitis via colonoscopy in 2002 by my pediatric gastroenterologist, Dr. Markowitz at North Shore University Hospital. I was very sick at the time of my diagnosis and so I was put on 60 mg. of Prednisone (a corticosteroid) and was also prescribed Asacol, a 5-ASA or mesalamine drug. I would take 16 Asacol pills daily (4 pills, 4 times a day), though thanks to the CCFA and strides made in the field of research, Asacol was recently condensed and is now given as 1 pill, once per day. I was also given prescription Iron to treat my anemia and a prescribed form of Folic Acid as Ulcerative Colitis patients are known to have chronically-low Folic Acid levels.
Thanks to Prednisone, I was able to achieve remission from U.C. within two weeks of my diagnosis, although I had lost 20 pounds and was very weak so it took quite a bit longer to gain my strength back. I was slowly weaned off of the Prednisone over a period of 4 months and felt well for that length of time. Unfortunately, once I was off the Prednisone, the Asacol was unable to keep me in remission on its own and so my doctor added Colazal (Balzalazide), another 5-ASA agent to my regimen. This added another 10 pills daily, and I believe at this point I was up to around 31 pills/day. The Colazal didn't work. Instead of taking me off of the 5-ASA agents, another drug was added. At this point (about 8 months after my diagnosis) I was given 6MP (mercaptopurine), a drug used more often in the treatment of leukemia that required biweekly blood tests to assure my white blood cell count remained in a healthy range. As an important side note, Ulcerative Colitis is an autoimmune disease, meaning your immune system attacks itself. Therefore, the treatment for Ulcerative Colitis necessarily requires the suppression of your immune system, and so these treatments lower your white blood cell count and inhibit your body's natural ability to fight off infections. I was able to achieve intermittent remission with 6MP, but was left on the 5-ASA agents for 3 years.
During a routine visit to my gastroenterologist in Maine while I was in college, my doctor found high amounts of protein in my urine which is symptomatic of compromised kidney function. I was immediately sent to a nephrologist who deduced that the damage done to my kidneys was caused by the 5-ASA agents. Now, I must explain that this is a rare complication of 5-ASA drugs, though it does happen. 5-ASA are the most mild and least risky treatments used for U.C. and those that are able to obtain remission on 5-ASA agents with no serious side effects are very lucky.
For me, 5-ASA agents were eternally taken off the radar. I was no longer a candidate for them, but because of their very limited efficacy in treatment of my U.C., I did not find this news to be particularly troublesome. I was now onto a cocktail of 6MP and high doses of Prednisone (the Prednisone was taken sporadically, but I spent more time on them than off).
In conclusion, 5-ASA drugs are relatively harmless in comparison to other U.C. treatment options and if they work for you...stick with them!
And, oh, I turned those pictures around from yesterday as I know it was irking some of you!
Wednesday, May 4, 2011
Scars
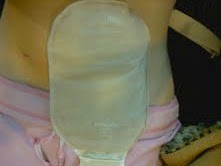
I want to document my scars at this point for several reasons. Before I went into surgery I was curious to know the length/width and overall appearance of the scars that were soon to become a permanent part of me and so I would like to show other panproctocolectomy patients what they can expect. I would also like to document them for myself so I can watch the progression and be able to look back and appreciate the body's healing process. In order to capture my scars, I will also need to show my ostomy appliance and so I will give a brief explanation of how that works:
The ostomy is a two-part system. The "flange" is the part that sticks to my body. A whole is cut in this system that is sized to fit perfectly around my stoma (my small intestine that is pulled through the skin). The bag clicks onto the flange to cover the ileostomy and collect waste. There is no smell and the bag is fairly easy to hide. I wear beige-colored bags, so you will not see my ileostomy/stoma in the pictures. If anyone has any questions about the ileostomy, please feel free to ask. I know I had a million questions about it before I went into surgery so I would be happy to help anyone out. Please note that an "ileostomy" (a stoma that uses the small intestine) is different from a "colostomy" (a stoma that uses the large intestine) and they function in very different ways.
The appearance of my abdomen will change after my second "takedown" surgery that will hopefully occur around the last week of June or first week of July. The ileostomy will be reversed and so instead of the ostomy appliance I will simply have a scar from where it used to be.
For now, this is what my abdomen looks like (5 weeks post-op). The scar on the left side of my abdomen is from the sump that was draining fluid from my abdominal cavity during surgery until a few days after surgery. The top photograph shows the ostomy. The bottom two photographs show my scar and the scars from the staples. The scar continues quite a bit further down my abdomen to the end of the pubic bone and the total length is 18 cm. You will notice some post-operative swelling on the left side of my abdomen that is actually muscular inflammation. It is slowly going down, but is still fairly visible 5 weeks later.
The ostomy is a two-part system. The "flange" is the part that sticks to my body. A whole is cut in this system that is sized to fit perfectly around my stoma (my small intestine that is pulled through the skin). The bag clicks onto the flange to cover the ileostomy and collect waste. There is no smell and the bag is fairly easy to hide. I wear beige-colored bags, so you will not see my ileostomy/stoma in the pictures. If anyone has any questions about the ileostomy, please feel free to ask. I know I had a million questions about it before I went into surgery so I would be happy to help anyone out. Please note that an "ileostomy" (a stoma that uses the small intestine) is different from a "colostomy" (a stoma that uses the large intestine) and they function in very different ways.
The appearance of my abdomen will change after my second "takedown" surgery that will hopefully occur around the last week of June or first week of July. The ileostomy will be reversed and so instead of the ostomy appliance I will simply have a scar from where it used to be.
For now, this is what my abdomen looks like (5 weeks post-op). The scar on the left side of my abdomen is from the sump that was draining fluid from my abdominal cavity during surgery until a few days after surgery. The top photograph shows the ostomy. The bottom two photographs show my scar and the scars from the staples. The scar continues quite a bit further down my abdomen to the end of the pubic bone and the total length is 18 cm. You will notice some post-operative swelling on the left side of my abdomen that is actually muscular inflammation. It is slowly going down, but is still fairly visible 5 weeks later.
Tuesday, May 3, 2011
Spreading Hope
I noticed on facebook that today is Iris' one-year anniversary (from the day she had her takedown surgery) and she has posted a new video that marks her progress and success with her J-Pouch. She also posted another video last month about her scars and what they look like 11-months post-takedown surgery. Her scars look very much like mine, so I am hoping that mine will heal as well as her's have!
Iris has been a huge source of inspiration for not only me, but many other Ulcerative Colitis sufferers and panproctocolectomy patients around the world. I have had a couple of people reach out to me, asking if I would be willing to answer questions or speak with others about my experiences or to answer questions about U.C. or my surgeries. The answer is an emphatic YES! I would be very, very happy to speak with anyone at all and answer any questions they might have....I find it comforting and encouraging myself to know that there are others out there like me and that I can perhaps help them in some way. I am going to begin documenting my progress through photographs, to give people going through this (or those that are curious) an idea of what they can expect.
One other note of great news is that it seems as though Iris' band and my brother Mark's band are going to team up in August to play a show to benefit the Crohn's and Colitis Foundation of America (CCFA). So please check out Iris' new links and her band's website, and also please check out Mark's band's website as well! More details on this to follow and here are the links:
Iris' videos:
http://www.youtube.com/user/IrisUCVlog#p/u/5/vROdqr7lI0o
(anniversary video isn't on YouTube yet, I'll post it when it is)
Iris' band:
http://roadsband.com/
Mark's band:
http://thealphabetsband.bandcamp.com/album/cats-dogs
Iris has been a huge source of inspiration for not only me, but many other Ulcerative Colitis sufferers and panproctocolectomy patients around the world. I have had a couple of people reach out to me, asking if I would be willing to answer questions or speak with others about my experiences or to answer questions about U.C. or my surgeries. The answer is an emphatic YES! I would be very, very happy to speak with anyone at all and answer any questions they might have....I find it comforting and encouraging myself to know that there are others out there like me and that I can perhaps help them in some way. I am going to begin documenting my progress through photographs, to give people going through this (or those that are curious) an idea of what they can expect.
One other note of great news is that it seems as though Iris' band and my brother Mark's band are going to team up in August to play a show to benefit the Crohn's and Colitis Foundation of America (CCFA). So please check out Iris' new links and her band's website, and also please check out Mark's band's website as well! More details on this to follow and here are the links:
Iris' videos:
http://www.youtube.com/user/IrisUCVlog#p/u/5/vROdqr7lI0o
(anniversary video isn't on YouTube yet, I'll post it when it is)
Iris' band:
http://roadsband.com/
Mark's band:
http://thealphabetsband.bandcamp.com/album/cats-dogs
Subscribe to:
Comments (Atom)